White blood cells, also known as leukocytes, are the frontline soldiers of your immune system, tirelessly working to protect your body from infection and disease.
These microscopic defenders circulate through your bloodstream, ready to identify, target, and neutralize foreign invaders like bacteria, viruses, and other harmful pathogens.
In fact, your body is a remarkable factory, producing nearly 100 billion of these cells every single day to keep you healthy.
Understanding your white blood cells is crucial because their numbers can provide a vital window into your overall health.
A count that is too high or too low can be the first sign of a hidden infection, an underlying inflammatory condition, or other medical issues that require attention.
This comprehensive guide will walk you through everything you need to know about your immune army.
We will explore the different types of white blood cells, what they do, what normal levels look like, and what it means when your count is outside the typical range.
Read on to become an expert on this essential part of your body’s defense system.
In This Article
What Are White Blood Cells (Leukocytes)?
At its core, a white blood cell is a specialized cell of the immune system. The scientific name for these cells is leukocytes, derived from the Greek words ‘leukos’ (white) and ‘kytos’ (cell).
Unlike red blood cells, which are responsible for transporting oxygen, the primary mission of white blood cells is defense. They are your body’s internal security force, constantly patrolling your blood and tissues for signs of trouble.
The Role of White Blood Cells in Your Immune System
Think of your immune system as a highly coordinated army. In this army, white blood cells are the diverse and specialized troops.
When a pathogen—such as a virus, bacterium, or fungus—invades your body, or when your own cells become damaged or cancerous, your white blood cells spring into action. They act as both sentinels and soldiers.
As sentinels, they travel through your bloodstream and can even squeeze through blood vessel walls to enter tissues, locating the site of an injury or infection.
Once they identify an invader, they act as generals, sending chemical signals to recruit more white blood cells to the area. This coordinated response is what causes the inflammation, redness, and swelling you often see around a cut or infection.
As soldiers, they directly attack and destroy the invaders, clean up dead cells, and produce antibodies to prevent future infections from the same pathogen.
White Blood Cells vs. Red Blood Cells: What’s the Difference?
While both are crucial components of your blood, white and red blood cells have vastly different roles, structures, and numbers. The most significant difference lies in their function: red blood cells carry oxygen, while white blood cells fight infection.
Numerically, they are not even close. White blood cells make up only about 1% of your total blood volume. For every one white blood cell, there are hundreds of red blood cells.
Structurally, red blood cells are biconcave discs without a nucleus, which maximizes their oxygen-carrying capacity.
In contrast, all white blood cells contain a nucleus, which holds the genetic material necessary for their complex functions of identifying and fighting pathogens.
The Anatomy of a White Blood Cell: A Closer Look
To truly appreciate these immune defenders, it helps to understand where they come from and what they’re made of. Their formation and structure are perfectly tailored to their protective role.
Where Are White Blood Cells Formed and Stored?
The vast majority of white blood cells originate from hematopoietic stem cells in the soft, spongy tissue inside your bones, known as the bone marrow. These remarkable stem cells have the potential to develop into any type of blood cell.
While most WBCs are born in the bone marrow, some types mature and specialize elsewhere. For example, a specific type of lymphocyte known as a T cell travels to the thymus gland (a small organ behind your breastbone) to mature.
Other lymphocytes, called B cells, mature in the bone marrow but are often found in lymph nodes and the spleen, where they are ready to respond to infections.
What Do White Blood Cells Look Like?
Despite their name, white blood cells are actually colorless in their natural state. They only appear white when collected in large numbers.
When viewed under a microscope, they are translucent. To make them visible for analysis, scientists use special dyes that stain different parts of the cell, often giving them a light purple or pink appearance.
They are generally round and, unlike red blood cells, possess a large, distinct nucleus at their center.
How Many White Blood Cells Do You Have?
As mentioned, white blood cells constitute about 1% of your blood, but this small percentage represents a massive number of cells. A healthy adult produces around 100 billion white blood cells every day.
This constant production is necessary because WBCs have a relatively short lifespan, ranging from a few hours to several days, especially when they are actively fighting an infection.
Their numbers are measured in cells per microliter of blood, a topic we’ll explore in detail later.
What Are the 5 Types of White Blood Cells and Their Functions?
The “white blood cell army” is not a single entity but a team of five distinct types of cells, each with a specialized role.
This division of labor allows your immune system to mount a sophisticated and targeted defense against a wide variety of threats.
The five major types are neutrophils, lymphocytes, monocytes, eosinophils, and basophils.
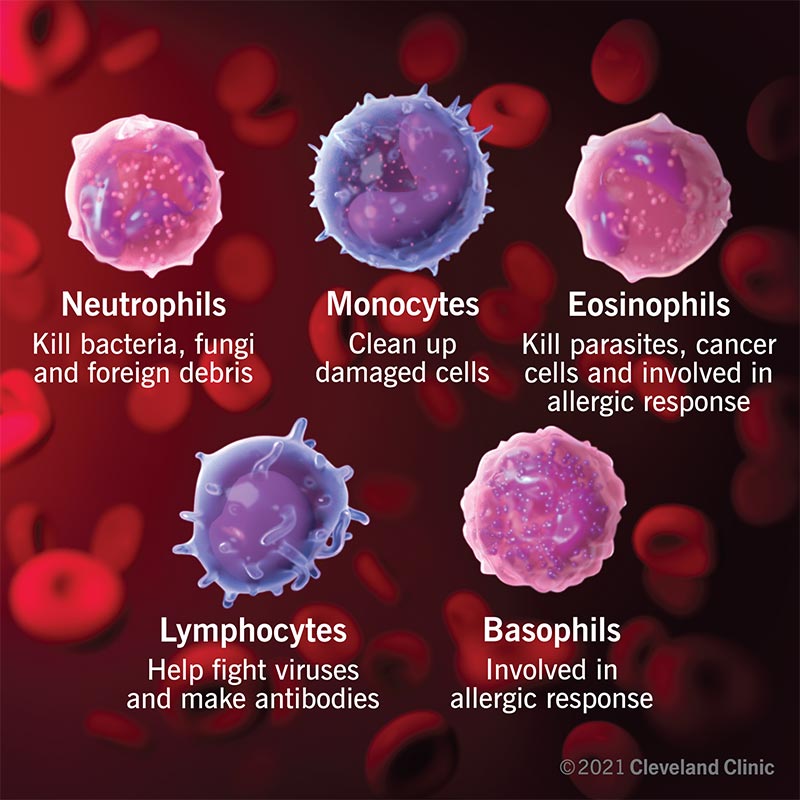
1. Neutrophils
Neutrophils are the most abundant type of white blood cell, making up 55% to 70% of your total count.
They are the rapid-response force and first responders to the site of an infection, particularly bacterial or fungal infections.
They are phagocytes, meaning they engulf and digest harmful microorganisms and debris.
The pus that forms in an infected wound is largely composed of dead neutrophils that have sacrificed themselves to clear the infection.
2. Lymphocytes (T cells, B cells, and Natural Killer cells)
Lymphocytes are the intelligence agency of your immune system and account for 20% to 40% of your WBCs.
They are crucial for creating “memory” of past infections. There are three main types:
- B cells: These cells produce proteins called antibodies. Antibodies are like custom-made keys that lock onto specific invaders (antigens), marking them for destruction by other immune cells. B cells are central to long-term immunity.
- T cells: These cells have multiple roles. Some “helper” T cells coordinate the immune response by activating other cells, while “killer” T cells directly attack and destroy your body’s own cells that have been infected by viruses or have become cancerous.
- Natural Killer (NK) cells: These cells are part of your innate immune system and can kill tumor cells and virus-infected cells without needing to have “met” them before.
3. Monocytes
Monocytes are the largest type of white blood cell and make up 2% to 8% of the count. They are the “clean-up crew”.
After circulating in the bloodstream for a day or two, they migrate into tissues and mature into macrophages.
As macrophages, they are powerful phagocytes that devour dead cells, cellular debris, and pathogens.
They also play a key role in presenting pieces of pathogens to T cells, helping to initiate a more specific immune response.
4. Eosinophils
Eosinophils are specialized warriors, comprising 1% to 4% of your WBCs. Their primary roles are fighting parasitic infections and playing a part in allergic reactions.
They release potent toxins to destroy parasites like worms. They are also heavily involved in the inflammation associated with conditions like asthma and allergies.
High levels of eosinophils are often a sign of an allergic reaction or a parasitic infection.
5. Basophils
Basophils are the rarest type of white blood cell, making up less than 1% of the total count. Though few in number, they are powerful.
They are best known for their role in allergic responses. When they detect an allergen, they release histamine and other chemicals.
This is what causes the classic allergy symptoms: sneezing, runny nose, watery eyes, and itching. This response, while annoying, is designed to help expel the perceived threat from your body.
Understanding the White Blood Cell (WBC) Count Test
A white blood cell (WBC) count is a simple blood test that measures the number of leukocytes in your blood. It’s a fundamental diagnostic tool that provides a snapshot of your immune system’s activity.
This test is rarely performed alone; it is almost always part of a broader panel called a complete blood count (CBC).
Why Would a Doctor Order a WBC Count?
Your doctor might order a CBC, including a WBC count, for several reasons:
- Routine Health Check: It’s often included in an annual physical to get a baseline of your overall health.
- Diagnosing an Infection: If you have symptoms like fever, chills, or body aches, a WBC count can help confirm if your body is fighting an infection.
- Identifying Underlying Conditions: An abnormal count can be a clue to undiagnosed medical conditions, such as autoimmune diseases, immune deficiencies, or blood disorders like leukemia.
- Monitoring Treatment: For patients undergoing treatments like chemotherapy or radiation, regular WBC counts are essential to monitor how the treatment is affecting the immune system and bone marrow.
The Complete Blood Count (CBC) and WBC Differential
A standard WBC count gives you the total number of white blood cells. However, doctors often need more detail.
For this, they order a WBC count with differential. This test breaks down the total count into the percentages of each of the five types of white blood cells.
This level of detail is incredibly valuable. For example, a high total WBC count with high neutrophils suggests a bacterial infection, while a high count with high lymphocytes might point to a viral infection.
How to Prepare for a WBC Count Test
The good news is that a WBC count test requires no special preparation. You do not need to fast or alter your daily routine. The test involves a simple blood draw, usually from a vein in your arm, which is then sent to a laboratory for analysis.
What Medications Can Affect Your WBC Count?
It’s very important to tell your healthcare provider about all medications you are taking, including over-the-counter drugs and supplements.
Certain medications can significantly raise or lower your white blood cell count, which could lead to a misinterpretation of your results. Medications known to affect WBC counts include:
- Corticosteroids: Can increase your WBC count.
- Antibiotics: Some can lower your WBC count.
- Chemotherapy drugs: Routinely lower WBC counts by suppressing bone marrow.
- Diuretics, anticonvulsants, and antihistamines: Can also influence the results.
What Is a Normal White Blood Cell Count Range?
A “normal” white blood cell count can vary based on several factors, including age, sex, and the specific reference ranges used by the laboratory performing the test.
However, generally accepted ranges provide a good guideline for what is considered healthy.
A typical normal white blood cell count range for adults is between 4,000 and 11,000 cells per microliter (μL) of blood.
Normal Ranges for Adults and Children
According to data from organizations like the Leukemia and Lymphoma Society (LLS), normal ranges can be broken down more specifically.
It’s important to note that pregnant individuals, newborns, and young children have different normal ranges.
| Age/Group | Normal WBC Range (cells per μL) |
|---|---|
| Adults assigned male at birth | 5,000 to 10,000 |
| Adults assigned female at birth (non-pregnant) | 4,500 to 11,000 |
| Children | 5,000 to 10,000 |
Note: Newborns and children under two may have significantly higher ranges, which is normal as their immune systems develop.
Normal Percentages for Each WBC Type
The WBC differential test provides the percentage of each type of cell. A deviation in these percentages can be just as significant as an abnormal total count.
| Type of White Blood Cell | Normal Percentage of Overall WBC Count |
|---|---|
| Neutrophils | 55–70% |
| Lymphocytes | 20–40% |
| Monocytes | 2–8% |
| Eosinophils | 1–4% |
| Basophils | 0.5–1% |
What Does a Low White Blood Cell Count (Leukopenia) Mean?
A low white blood cell count, medically termed leukopenia, is diagnosed when your count falls below 4,000 cells per microliter. This condition indicates that your body may not have enough defenses to fight off infections, leaving you more vulnerable to getting sick.
Common Causes of a Low WBC Count
Leukopenia is not a disease itself but a sign of an underlying issue. The causes can range from temporary viral infections to serious medical conditions. Common causes include:
- Bone Marrow Problems: Since the bone marrow is the WBC factory, any damage or failure can lead to low counts. This includes conditions like aplastic anemia or bone marrow suppression from cancer cells (e.g., leukemia).
- Cancer Treatments: Chemotherapy and radiation therapy are designed to kill rapidly dividing cells. While they target cancer, they also damage the bone marrow, leading to a sharp drop in WBCs.
- Autoimmune Disorders: Conditions like lupus can cause the immune system to mistakenly attack and destroy its own white blood cells.
- Severe Infections: Overwhelming infections, such as sepsis, can use up white blood cells faster than the body can produce them.
- Viral Infections: Some viruses, including HIV/AIDS, directly attack and destroy lymphocytes.
- Medications: Besides chemotherapy, other drugs like certain antibiotics and diuretics can cause leukopenia as a side effect.
- Nutritional Deficiencies: A severe deficiency in vitamins like B12 or folate can impair the body’s ability to produce WBCs.
- Spleen or Liver Disease: An enlarged spleen can trap and destroy blood cells, leading to lower counts in circulation.
Understanding Neutropenia: The Most Common Type of Leukopenia
Because neutrophils make up the largest portion of your white blood cells, a low overall WBC count is often due to a low number of neutrophils.
This specific condition is called neutropenia. Having neutropenia significantly increases your risk of bacterial infections, and your doctor may recommend extra precautions, like wearing a mask in public, to protect you.
Symptoms Associated with a Low WBC Count
Leukopenia itself doesn’t cause symptoms. The symptoms you experience are usually from the infections that your body can’t fight off. These include:
- Fever and chills
- Frequent or recurring infections
- Body aches and fatigue
- A persistent cough or shortness of breath
- Wounds that are red, swollen, ooze pus, or won’t heal
What Does a High White Blood Cell Count (Leukocytosis) Mean?
A high white blood cell count, or leukocytosis, is generally defined as a count above 11,000 cells per microliter.
Most often, this is a normal and healthy sign that your immune system is doing its job—ramping up production to fight an infection or respond to inflammation.
Common Causes of a High WBC Count
An elevated WBC count can be caused by a wide range of factors, from the body’s normal response to stress to serious diseases.
Acute (Short-Term) Causes:
- Infections: This is the most common cause. Both bacterial infections (like sepsis) and viral infections (like mononucleosis) trigger a surge in WBC production.
- Inflammation: Any inflammatory condition, from an injury or burn to a flare-up of an autoimmune disorder like rheumatoid arthritis, can raise your count.
- Physical or Emotional Stress: Intense exercise, surgery, or severe emotional stress can temporarily increase WBC levels.
- Allergies and Asthma: Allergic reactions cause an increase in specific WBCs, particularly eosinophils and basophils.
- Medications: Drugs like corticosteroids and epinephrine can cause leukocytosis.
- Pregnancy: It is normal for the WBC count to be elevated during the later stages of pregnancy and labor.
Chronic (Long-Term) Causes:
- Smoking: Chronic inflammation caused by smoking is a common reason for a persistently high WBC count.
- Blood Cancers: Cancers of the blood and bone marrow, such as leukemia and lymphoma, lead to the uncontrolled production of abnormal white blood cells.
- Chronic Inflammatory Conditions: Diseases like inflammatory bowel disease (IBD) or certain types of arthritis can cause long-term elevation.
- Obesity: Chronic low-grade inflammation associated with obesity can also lead to a higher baseline WBC count.
Symptoms Associated with a High WBC Count
Much like leukopenia, leukocytosis itself rarely causes symptoms. The symptoms are typically related to the underlying condition causing the high count.
For example, if an infection is the cause, you’ll have a fever and feel unwell. If leukemia is the cause, you might experience fatigue, unexplained weight loss, and easy bruising.
How Are White Blood Cell Disorders Diagnosed and Treated?
An abnormal WBC count is a starting point, not a final diagnosis. If your count is high or low, your doctor will act as a detective, using your medical history, symptoms, and further tests to find the root cause.
Diagnostic Tests Beyond the CBC
After an abnormal CBC result, your doctor may order additional tests:
- Blood Smear: A drop of your blood is spread on a slide and examined under a microscope. This allows a pathologist to visually inspect the different types of white blood cells for abnormalities in shape or size.
- White Blood Cell Scan: This imaging test is used to locate hidden infections or abscesses. It involves drawing your blood, separating the WBCs, tagging them with a safe radioactive substance, and reinjecting them. A special camera then tracks where the tagged cells accumulate in your body.
- Bone Marrow Biopsy: If a serious blood disorder or cancer is suspected, your doctor may need to take a small sample of your bone marrow, usually from the hip bone, for analysis. This provides the most definitive information about blood cell production.
Common Treatment Approaches
Treatment is always directed at the underlying cause of the abnormal WBC count, not the count itself. The approach varies widely based on the diagnosis:
- For Infections: Antibiotics for bacterial infections or antiviral medications for viral ones will help the body clear the infection, allowing the WBC count to return to normal.
- For Nutritional Deficiencies: Taking vitamin supplements (like B12 or folate) and making dietary changes can correct the deficiency and restore normal WBC production.
- For Drug-Induced Issues: Your doctor may adjust the dosage of a medication or switch you to a different one.
- For Serious Disorders: Conditions like leukemia or bone marrow failure require specialized treatments, which can include chemotherapy, blood transfusions, or a stem cell transplant to replace the diseased bone marrow.
When to See a Doctor
You should contact your healthcare provider if you experience persistent symptoms associated with abnormal WBC counts, such as a fever that won’t go away, frequent infections, unexplained fatigue, or wounds that don’t heal.
These can be signs that your immune system is struggling or overactive.
How Can You Support Healthy White Blood Cell Levels?
While you can’t directly control your WBC count, you can adopt a healthy lifestyle that supports a robust and balanced immune system.
This involves reducing your risk of infection and providing your body with the nutrients it needs to function optimally.
Lifestyle and Hygiene Practices
The first line of defense is preventing infections from taking hold in the first place. Simple habits can make a big difference:
- Practice Good Hygiene: Wash your hands frequently with soap and water, especially before eating and after being in public places.
- Avoid Crowds When Sick: If you know your immune system is compromised, try to avoid large gatherings to reduce your exposure to germs.
- Manage Stress: Chronic stress can suppress the immune system. Incorporate stress-reducing activities like meditation, yoga, or hobbies into your routine.
- Get Enough Sleep: Sleep is when your body repairs itself and produces immune cells. Aim for 7-9 hours of quality sleep per night.
The Role of Diet and Nutrition
A balanced diet is essential for building the components of your immune system. While no single food is a magic bullet, a diet rich in certain nutrients is key.
It’s important to include a good source of protein, as the amino acids in protein are the building blocks for white blood cells and antibodies.
Additionally, two vitamins are critical for WBC production: Vitamin B12 and folate. These are found in foods like meat, fish, eggs, dairy, and leafy green vegetables.
Can Supplements Boost Your White Blood Cells?
Many people wonder if supplements can help. While a balanced diet is always best, some research suggests certain vitamins and minerals are important for immune function.
These include vitamins C and E, zinc, and selenium. However, it’s crucial to talk with a doctor before starting any supplements, especially if you are undergoing treatment for a medical condition, as they can sometimes interfere with medications.
Frequently Asked Questions
How many white blood cells are produced daily?
A healthy adult body is a prolific factory, producing approximately 100 billion new white blood cells every single day. This rapid production is necessary to replenish cells that have been used up fighting infections or have reached the end of their short lifespan.
Can stress cause a high white blood cell count?
Yes, both physical and emotional stress can cause a temporary increase in your white blood cell count. This is part of the body’s “fight or flight” response. The elevation is usually mild and short-lived, returning to normal once the stressor is removed.
What is the difference between leukopenia and neutropenia?
Leukopenia refers to a low count of all types of white blood cells combined. Neutropenia is more specific; it refers to a low count of only neutrophils. Since neutrophils are the most common WBC, severe neutropenia often leads to a diagnosis of leukopenia.
Is a WBC count of 12,000 high?
Yes, a count of 12,000 cells/μL is considered mildly high (leukocytosis), as the typical upper limit is 11,000. This is often a sign that your body is fighting a minor infection or is experiencing inflammation. Your doctor will interpret this result in the context of your symptoms.
What foods can help increase white blood cells?
No specific diet is proven to increase WBC production, but a balanced diet is crucial. Focus on adequate protein (for amino acid building blocks) and foods rich in Vitamin B12 and folate, such as lean meats, fish, dairy, and leafy greens, which are essential for cell production.
Does smoking affect white blood cell count?
Yes, smoking is a well-known cause of chronic, long-term leukocytosis. The constant inflammation and tissue damage caused by inhaling smoke puts the immune system on high alert, leading to a persistently elevated white blood cell count, which is not a healthy state.
How long does it take for a WBC count to return to normal?
This depends entirely on the cause. After a minor infection, it may return to normal within days or a week. If it’s due to a medication, it should normalize after the drug is stopped. For more serious conditions, it depends on the effectiveness of the treatment.
What is a WBC differential test?
A WBC differential test breaks down your total white blood cell count into the specific numbers and percentages of each of the five types: neutrophils, lymphocytes, monocytes, eosinophils, and basophils. This provides a much more detailed picture of your immune response.
Your Immune Army: A Final Word
Your white blood cells are a dynamic and essential part of your health, serving as your personal, ever-vigilant army against illness.
Understanding their function and what their numbers mean can empower you to take a more active role in your health.
An abnormal count is not a reason to panic, but rather a valuable signal from your body that warrants a conversation with your healthcare provider.
By practicing good hygiene, eating a nutritious diet, and managing stress, you can provide the best possible support for your immune system.
If you have concerns about your health or symptoms of an infection, don’t hesitate to reach out to a medical professional.
They can help you interpret what your body is telling you and ensure your immune army stays strong.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. The information contained herein is not a substitute for, and should never be relied upon for, professional medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.

