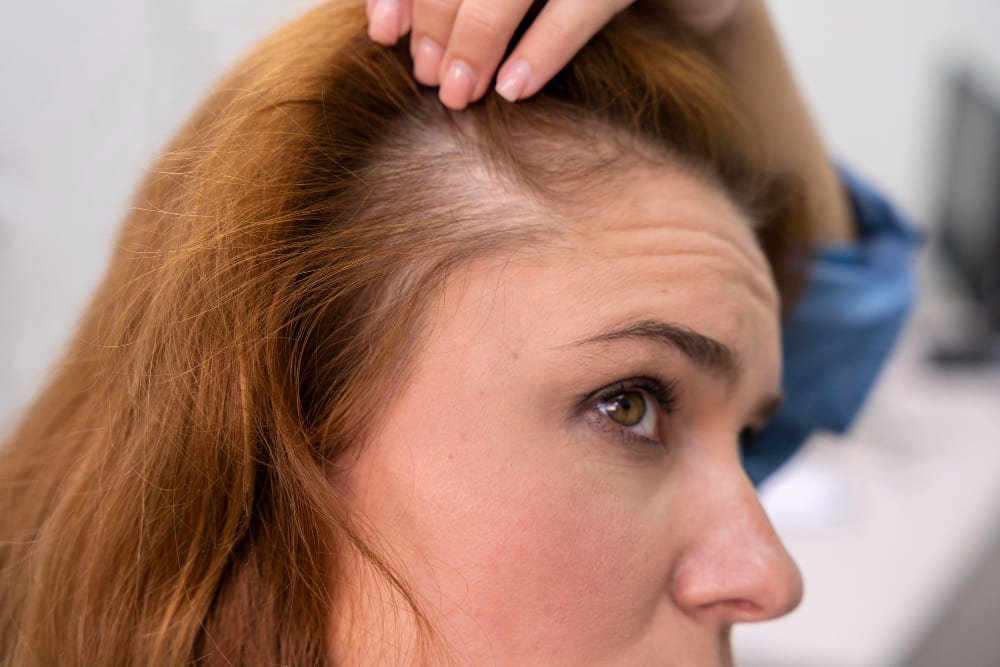
The primary cause of hair loss in women is androgenetic alopecia, a genetic condition also known as female pattern hair loss.
However, numerous other factors, including hormonal shifts, medical conditions, stress, and nutritional deficiencies, can also trigger significant hair thinning.
In fact, studies show that over 50% of women will experience noticeable hair loss at some point in their lives, a reality that can be both distressing and confusing.
Understanding the specific reason behind your hair loss is the critical first step toward finding an effective solution.
This comprehensive guide delves into the science behind why women lose their hair, exploring everything from the most common culprits to the less obvious triggers.
We will break down the different types of alopecia, explain the diagnostic process, and provide an in-depth look at the latest evidence-based treatments.
By the end of this article, you will have a clear roadmap to help you address your concerns and take control of your hair health.
In This Article
What Is Considered Normal Hair Loss vs. a Problem?
Every day, the average person sheds between 50 and 100 hairs.
This is a normal part of the hair’s life cycle and usually goes unnoticed because new hairs are constantly growing in to replace the ones that are lost.
This natural process is part of a delicate balance within the hair follicle.
Hair loss in women becomes a concern when this balance is disrupted—either because shedding increases significantly, or because new hair growth slows down or stops.
This condition, known medically as alopecia, can manifest in various ways, from a general thinning all over the scalp to distinct bald patches.
Understanding the Hair Growth Cycle
To understand hair loss, it’s helpful to know how hair grows. Each hair on your head goes through three distinct phases:
- Anagen (Growing Phase): This is the active growth phase, which can last anywhere from two to eight years. At any given time, about 85-90% of the hair on your scalp is in this phase.
- Catagen (Transition Phase): A short, transitional phase lasting two to three weeks, where the hair follicle shrinks and detaches from its blood supply.
- Telogen (Resting Phase): This phase lasts for about two to four months. The hair doesn’t grow but remains attached to the follicle while a new hair begins to form underneath. At the end of this phase, the old hair sheds to make way for the new one.
Disruptions to this cycle are at the heart of most types of hair loss in women.
For example, a major stressor can push a large number of hairs prematurely into the telogen phase, leading to widespread shedding a few months later.
What Are the Main Types of Hair Loss in Women?
While many people think of a receding hairline when they hear “hair loss”, the presentation in women is often different.
Identifying the pattern and type of hair loss is a key part of diagnosis. Here are the most common types affecting women.
Androgenetic Alopecia (Female Pattern Hair Loss)
This is the most common cause of hair loss in women, affecting an estimated 30 million women in the United States alone, according to MedlinePlus Genetics.
It’s a hereditary condition that, contrary to its name, doesn’t always involve high levels of androgens (male hormones).
Instead, it’s often due to a heightened sensitivity of the hair follicles to these hormones.
- Pattern: Typically starts with a gradual thinning at the part line, which slowly widens over time. This is often described as a “Christmas tree” pattern. Unlike male pattern baldness, it rarely leads to a receding hairline or total baldness.
- Mechanism: Hair follicles shrink in a process called follicular miniaturization, producing progressively shorter, finer hairs until they stop growing altogether.

Female-pattern baldness typically starts with thinning along the part line.
Telogen Effluvium
This is the second most common type of hair loss and is characterized by a sudden, diffuse shedding of hair from all over the scalp.
It occurs when a significant stressor pushes a large number of growing (anagen) hairs into the resting (telogen) phase simultaneously. About three to six months after the triggering event, these hairs begin to shed.
- Triggers: Common causes include major surgery, significant emotional stress, childbirth (postpartum hair loss), rapid weight loss, high fever, or starting/stopping certain medications.
- Characteristics: The hair loss is temporary, and hair typically regrows within six to nine months once the underlying stressor is resolved.
Alopecia Areata
This is an autoimmune disease where the body’s immune system mistakenly attacks the hair follicles, causing hair to fall out in small, round, smooth patches.
It can affect the scalp, eyebrows, eyelashes, or any hair-bearing skin.
- Presentation: The sudden appearance of one or more coin-sized bald patches. The skin may feel itchy or slightly painful before the hair falls out.
- Prognosis: The course is unpredictable. Hair may regrow on its own and then fall out again. In some cases, it can progress to total scalp hair loss (alopecia totalis) or total body hair loss (alopecia universalis).
Traction Alopecia
This type of hair loss is caused by prolonged or repetitive tension on the hair follicles. It’s a mechanical issue, not a biological one, and is entirely preventable.
- Causes: Tight hairstyles such as braids, cornrows, tight ponytails, or hair extensions that pull on the hair roots for extended periods.
- Warning Signs: It often begins as small bumps around the hair follicles and progresses to hair breakage and loss, typically along the hairline. If the tension continues, the follicles can become permanently damaged, leading to irreversible hair loss.
Frontal Fibrosing Alopecia (FFA)
This is a form of scarring alopecia that causes slow, progressive hair loss and scarring along the frontal hairline and eyebrows.
It primarily affects postmenopausal women, and its cause is unknown, though an autoimmune or hormonal link is suspected.
- Symptoms: A receding hairline that moves backward in a band-like pattern, often accompanied by loss of eyebrow hair. The affected skin may look pale or mildly scarred.
- Importance of Early Treatment: Because it is a scarring alopecia, the hair loss is permanent. Early diagnosis and treatment are crucial to halt its progression.

Frontal fibrosing alopecia causes a receding hairline and is a type of scarring alopecia.
Is Hair Loss in Women Primarily Genetic?
Yes, for many women, genetics is the single most significant factor. Female pattern baldness, or androgenetic alopecia, is a hereditary condition.
If your mother, father, or other close relatives experienced hair thinning, your risk is significantly higher.
However, the genetics of hair loss are complex and not fully understood. It’s not as simple as inheriting a single “baldness gene”.
Research suggests that multiple genes are involved, and you can inherit them from either side of your family. These genes can influence:
- The age at which hair loss begins.
- The rate and extent of the thinning.
- The sensitivity of your hair follicles to dihydrotestosterone (DHT), a byproduct of testosterone that is a key driver in shrinking follicles.
Even with a genetic predisposition, environmental and hormonal factors often play a crucial role in triggering or accelerating hair loss in women. This is why two sisters with the same genetic background might experience very different patterns of hair loss.
While you can’t change your genes, understanding your family history can help you and your doctor identify the likely cause of your hair loss early and begin preventative treatments to preserve the hair you have.
How Do Hormones Cause Hair Loss in Women?
Hormones are powerful chemical messengers that regulate countless bodily functions, including hair growth. When hormone levels fluctuate, it can have a direct and often dramatic impact on the hair cycle.
This is a major reason why hair loss in women is so common during certain life stages.
Pregnancy and Postpartum
During pregnancy, high levels of estrogen prolong the anagen (growth) phase of the hair cycle.
This means fewer hairs enter the resting phase and shed, resulting in hair that often feels thicker and more voluminous. However, this is temporary.
After childbirth, estrogen levels drop sharply. This sudden hormonal shift triggers a massive number of hairs to enter the telogen (resting) phase all at once.
A few months later, typically around three to six months postpartum, this leads to a condition called postpartum telogen effluvium, where women experience significant shedding.
While alarming, this type of hair loss is almost always temporary, and hair fullness usually returns by the baby’s first birthday.
Menopause
Menopause is another period of major hormonal upheaval. As a woman approaches menopause, levels of estrogen and progesterone decline. This has two main effects on hair:
- Slower Growth: The anagen phase shortens, so hair grows more slowly and becomes finer.
- Increased Androgen Effect: The decline in female hormones allows androgens (like testosterone) to have a more pronounced effect on hair follicles. This can unmask or accelerate underlying female pattern baldness, leading to noticeable thinning at the crown and part line. According to Harvard Health Publishing, as many as two-thirds of postmenopausal women experience hair thinning or bald spots.
Thyroid Disorders
The thyroid gland produces hormones that are essential for regulating metabolism.
Both an overactive thyroid (hyperthyroidism) and an underactive thyroid (hypothyroidism) can disrupt the hair growth cycle and cause diffuse hair loss.
In fact, hair loss is often one of the first noticeable symptoms of a thyroid problem. The hair loss is typically spread across the entire scalp rather than in patches.
Fortunately, once the thyroid condition is successfully treated, the hair loss usually resolves.
What Medical Conditions Are Linked to Female Hair Loss?
Beyond hormonal imbalances, several underlying medical conditions can manifest as hair loss in women.
It’s often a sign that something else is going on in the body, making a proper medical evaluation essential.
Polycystic Ovary Syndrome (PCOS)
PCOS is a common endocrine disorder characterized by a hormonal imbalance that can lead to irregular periods, acne, weight gain, and often, hair loss.
Women with PCOS may produce higher levels of androgens, which can trigger or worsen female pattern baldness.
A 2023 review in the journal Metabolic Syndrome and Associated Comorbidities highlights hyperandrogenism in PCOS as a key contributor to follicular miniaturization.
Treating the underlying hormonal imbalance of PCOS is often a key part of managing the associated hair loss.
Autoimmune Diseases
In autoimmune conditions, the body’s immune system attacks its own tissues.
- Alopecia Areata: As mentioned earlier, this is a direct autoimmune attack on the hair follicles.
- Lupus: This systemic autoimmune disease can cause widespread inflammation, which may lead to diffuse hair thinning. In some cases, it can also cause scarring alopecia, particularly in the form of discoid lupus, where lesions on the scalp destroy hair follicles permanently.
Scalp Infections
Infections on the scalp can invade the hair follicles and skin, leading to inflammation and hair loss.
The most common is tinea capitis, or ringworm of the scalp. This fungal infection can cause scaly patches, broken hairs, and inflammation.
If not treated promptly with antifungal medication, it can lead to scarring and permanent hair loss.
Trichotillomania (Hair-Pulling Disorder)
This is a mental health condition characterized by a recurrent, irresistible urge to pull out hair from the scalp, eyebrows, or other areas of the body.
It results in patchy hair loss and can cause significant distress. Treatment typically involves therapy, such as cognitive-behavioral therapy, to address the underlying compulsion.
Can Stress Really Make Your Hair Fall Out?
Yes, a significant physical or emotional shock can absolutely cause hair loss. This type of hair loss is known as telogen effluvium.
It’s not the day-to-day stress of a busy job that causes it, but rather a major life event that disrupts the body’s equilibrium.
As confirmed by experts at the Mayo Clinic, high stress levels can push a large number of hair follicles into the telogen (resting) phase.
A few months after the stressful event, you may notice a sudden increase in shedding. Handfuls of hair might come out when you brush or wash it.
Common Triggers for Telogen Effluvium:
- Physical Stress: Major surgery, a serious illness (especially with a high fever), a car accident, or even rapid weight loss.
- Emotional Stress: The death of a loved one, a divorce, job loss, or another traumatic event.
- Hormonal Stress: Childbirth is a classic example of a major physical and hormonal event that triggers telogen effluvium.
The good news is that this type of hair loss in women is almost always temporary.
Once the stressor is removed and your body recovers, the hair cycle normalizes, and your hair will begin to grow back.
The regrowth process can take several months, but full recovery is the typical outcome.
Which Vitamin Deficiencies Cause Hair Loss?
Your hair follicles are among the most metabolically active cells in your body. To build strong, healthy hair, they require a steady supply of key nutrients.
A deficiency in certain vitamins and minerals can impair hair production and lead to thinning.
It’s crucial to note that, as a 2017 study in Dermatology Practical & Conceptual points out, taking supplements without a confirmed deficiency can be ineffective and even harmful.
Over-supplementation of nutrients like Vitamin A, Vitamin E, and selenium has been linked to increased hair loss. Always consult a doctor and get blood tests before starting any supplement regimen.
Key Nutrients for Hair Health:
- Iron: Iron deficiency (anemia) is a very common cause of hair loss in women, especially premenopausal women. Iron is essential for producing hemoglobin, which carries oxygen for the growth and repair of cells, including the cells that stimulate hair growth.
- Vitamin D: Low levels of Vitamin D are linked to alopecia. Vitamin D helps create new follicles—the tiny pores from which new hairs grow. Research suggests a link, and your doctor may recommend a supplement if your levels are low.
- Zinc: Zinc plays a vital role in hair tissue growth and repair. It also helps keep the oil glands around the follicles working properly. A deficiency can lead to hair loss.
- Protein: Hair is made almost entirely of protein. Not consuming enough protein can cause your body to ration it by shutting down non-essential functions like hair growth.
- B Vitamins: While biotin (B7) is widely marketed for hair growth, deficiency is rare. However, deficiencies in other B vitamins like B12 can contribute to hair loss, particularly in vegetarians and vegans.
Can Medications or Medical Treatments Cause Hair Loss?
Yes, drug-induced hair loss is a well-documented side effect of many common medications.
The hair loss can be a form of telogen effluvium (temporary shedding) or, less commonly, anagen effluvium (a more immediate and severe loss that affects growing hairs).
Some of the most common culprits include:
- Chemotherapy Drugs: These powerful drugs are designed to kill rapidly dividing cancer cells, but they also affect other rapidly dividing cells, like those in hair follicles. This causes anagen effluvium, leading to rapid and extensive hair loss. The hair usually begins to grow back after treatment ends.
- Blood Pressure Medications: Certain types, such as beta-blockers and ACE inhibitors, have been linked to hair loss.
- Blood Thinners (Anticoagulants): Both heparin and warfarin can cause hair shedding.
- Antidepressants and Mood Stabilizers: Some medications used to treat depression and bipolar disorder can trigger telogen effluvium.
- High Doses of Vitamin A: Retinoids, often used for acne and anti-aging, can cause hair loss if taken in high doses.
If you suspect a medication is causing your hair loss, do not stop taking it. Talk to your doctor.
They can determine if the medication is the likely cause and may be able to prescribe an alternative.
What Lifestyle Factors Contribute to Hair Loss?
While genetics and medical conditions are major players, your daily habits can also have a significant impact on the health of your hair.
Hairstyling and Treatments
As mentioned with traction alopecia, excessive or harsh styling is a preventable cause of hair loss in women.
- Tight Styles: Constant pulling from tight braids, weaves, or ponytails can cause permanent damage to follicles.
- Heat Damage: Overuse of hot tools like flat irons and curling wands can weaken the hair shaft, making it brittle and prone to breakage. This isn’t true hair loss from the root, but it reduces volume and density.
- Chemical Treatments: Harsh chemical processes like bleaching, perming, and relaxing can damage the hair’s protein structure, leading to breakage. If chemicals cause a severe reaction on the scalp, they can also damage follicles.
Smoking
Smoking restricts blood flow to the tiny blood vessels that supply the hair follicles, depriving them of the oxygen and nutrients needed for healthy growth.
Some studies have shown a clear association between smoking and an increased risk of androgenetic alopecia.
Quitting smoking can improve circulation and benefit your overall health, including your hair.
Poor Diet and Extreme Weight Loss
A diet lacking in essential nutrients or a crash diet that leads to rapid weight loss can put immense stress on the body, often triggering telogen effluvium.
Ensuring a balanced diet rich in protein, iron, and other key vitamins is fundamental for maintaining healthy hair growth.
How Is the Cause of Hair Loss in Women Diagnosed?
Because there are so many potential causes, a thorough diagnosis from a healthcare provider, preferably a dermatologist, is essential.
A “one-size-fits-all” approach to treatment is ineffective, the strategy must target the specific cause.
The diagnostic process typically involves several steps:
- Detailed Medical and Family History: Your doctor will ask about your diet, medications, recent illnesses, stressors, and whether hair loss runs in your family.
- Physical Examination: The doctor will carefully examine your scalp to identify the pattern of hair loss, check for inflammation, scaling, or scarring, and assess the overall health of your hair.
- Pull Test: A simple test where the doctor gently tugs on a small section of hair to see how many strands come out. This helps gauge the severity of shedding.
- Blood Tests: These are crucial for ruling out underlying conditions. Common tests include a complete blood count (CBC), iron levels (ferritin), thyroid function tests, and sometimes hormone levels (like testosterone and DHEAS).
- Scalp Biopsy: In some cases, especially if a scarring alopecia is suspected, the doctor may take a tiny skin sample from your scalp (about 4mm) to examine the hair follicles under a microscope. This can provide a definitive diagnosis.
What Are the Most Effective Treatments for Hair Loss in Women?
Treatment for hair loss in women depends entirely on the diagnosis. The goal may be to regrow hair, prevent further loss, or both.
A 2023 review in Female-pattern hair loss: therapeutic update emphasizes that while many options exist, combination therapy often yields the best results.
| Treatment | How It Works | Best For | Considerations |
|---|---|---|---|
| Topical Minoxidil (Rogaine®) | Increases blood flow to follicles and prolongs the anagen (growth) phase. | Androgenetic Alopecia (FPHL) | Available OTC (2% and 5%). Must be used continuously to maintain results. Can cause scalp irritation or unwanted facial hair. |
| Oral Anti-Androgens (e.g., Spironolactone) | Blocks the effect of androgens on hair follicles. | FPHL, especially in women with PCOS or signs of high androgens. | Prescription only. Not for use during pregnancy. Can have side effects like dizziness or breast tenderness. |
| Low-Level Laser Therapy (LLLT) | Stimulates cellular activity in follicles to promote growth. | FPHL | FDA-cleared devices (combs, caps) for home use. Requires consistent, long-term use. Results can be variable. |
| Platelet-Rich Plasma (PRP) Therapy | Injects concentrated growth factors from your own blood into the scalp to stimulate follicles. | FPHL, Alopecia Areata | In-office procedure. Requires multiple sessions. Can be expensive and is not always covered by insurance. |
| Hair Transplantation | Surgically moves hair follicles from a dense area (like the back of the head) to a thinning area. | FPHL with stable donor hair. Scarring alopecias (if stable). | Surgical procedure with permanent results. Can be costly. Not all women are good candidates. |
| JAK Inhibitors | Blocks specific immune pathways that attack hair follicles. | Alopecia Areata | Newer class of oral medications (e.g., baricitinib). Highly effective but requires medical supervision due to potential side effects. |
Emerging Therapies
Research is constantly evolving. Oral minoxidil, used in low doses, is gaining popularity as an effective and convenient alternative to the topical version.
Additionally, as highlighted in a 2024 review in the Journal of Cosmetic Dermatology, combining therapies—such as using oral finasteride with topical minoxidil—is being explored to enhance efficacy, though its use in women requires careful consideration due to potential side effects.
How Can I Prevent or Stop Hair Loss?
While genetic hair loss isn’t entirely preventable, you can take steps to minimize preventable types of hair loss and promote a healthy environment for hair growth.
- Eat a Balanced Diet: Ensure you’re getting enough protein, iron, zinc, and vitamins. A diet rich in fruits, vegetables, lean proteins, and healthy fats supports overall health, including your hair.
- Be Gentle with Your Hair: Avoid harsh treatments and tight hairstyles that pull on your hair. Use a wide-toothed comb, especially on wet hair, and minimize the use of high-heat styling tools.
- Manage Stress: Incorporate stress-reducing activities into your routine, such as exercise, meditation, yoga, or spending time in nature. This can help prevent stress-induced telogen effluvium.
- Review Your Medications: Talk to your doctor about whether any medications you take could be contributing to hair loss and if alternatives are available.
- Stop Smoking: Quitting smoking improves circulation throughout your body, including to your scalp, which can help support healthier hair follicles.
- Address Health Issues Promptly: Don’t ignore symptoms of potential underlying conditions like thyroid disorders or anemia. Early diagnosis and treatment can reverse associated hair loss.
Frequently Asked Questions
What is the most common cause of hair loss in women?
The most common cause is androgenetic alopecia, also known as female pattern hair loss. It is a genetic condition that causes gradual thinning, typically starting at the part line, and affects over 30 million women in the U.S.
Can low iron cause hair loss in women?
Yes, iron deficiency is a very common and reversible cause of hair loss in women, particularly those who are premenopausal. Iron is essential for producing hemoglobin, which carries oxygen to your hair follicles for growth.
Will my hair grow back after telogen effluvium?
Yes, in most cases of telogen effluvium, the hair loss is temporary. Once the underlying stressor (like childbirth, illness, or stress) is resolved, the hair cycle normalizes, and hair typically regrows fully within 6 to 9 months.
What is the best vitamin for hair growth?
There is no single “best” vitamin. A balanced intake of several nutrients, including iron, vitamin D, zinc, and protein, is crucial. It’s best to get these from your diet and only supplement if a blood test confirms a deficiency.
How is female pattern baldness different from male pattern baldness?
In women, it typically presents as diffuse thinning over the crown and a widening part, while the frontal hairline is usually preserved. In men, it often starts with a receding hairline and thinning at the vertex, which can progress to complete baldness.
Can birth control pills cause hair loss?
Yes, some women may experience hair loss when starting or stopping certain types of hormonal birth control. This is usually a temporary form of telogen effluvium due to the hormonal shift. Pills with a higher androgen index are more likely to be culprits.
When should I see a doctor for hair loss?
You should see a doctor if you notice sudden or patchy hair loss, more shedding than usual, or if the hair loss is causing you distress. Early diagnosis is key to effective treatment and preventing permanent loss.
Is PRP therapy effective for hair loss in women?
PRP (Platelet-Rich Plasma) therapy has shown promising results for treating androgenetic alopecia. It uses growth factors from your own blood to stimulate hair follicles. Multiple sessions are usually needed, and results can vary between individuals.
Conclusion
Hair loss in women is a complex issue with a wide range of causes, from the unchangeable influence of genetics to the manageable effects of diet and stress.
The emotional impact can be significant, but it’s important to remember that you are not alone and that effective solutions are available.
The most critical action you can take is to seek a professional diagnosis from a dermatologist.
By identifying the specific cause of your hair loss, you can move forward with a targeted treatment plan that is right for you.
Whether it involves medical treatments like minoxidil, lifestyle adjustments, or nutritional support, taking proactive steps can help you manage your condition, prevent further thinning, and in many cases, restore your hair’s health and your confidence.
We encourage you to use this guide as a starting point for a conversation with your healthcare provider. Have you experienced hair loss? Share your story or questions in the comments below to connect with others on a similar journey.
This article is for informational purposes only and does not constitute medical advice. The information contained herein is not a substitute for, and should never be relied upon for, professional medical advice. Always talk to your doctor about the risks and benefits of any treatment.